Addressing vein pain and treating venous insufficiency to reduce the risk of blood clots may have more importance than ever in the era of COVID-19. While treatment is normally urged out of serious health concerns and improved quality of life, it takes on even more significance by eliminating factors that may complicate your health condition with the onset of the coronavirus variants.
Blood clots have become one of the many critical health problems associated with the coronavirus outbreak. American Heart Association research indicates that the virus affects the inner lining of blood vessels, posing potential blood clot risk to every part of the human body.
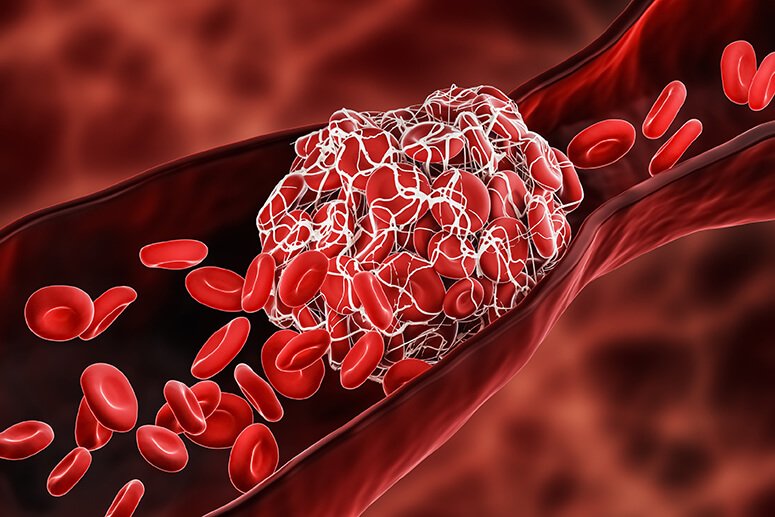
One of the characteristics of the coronavirus is believed to be thrombogenicity, the promotion of blood clotting. This may explain studies from Europe that put the incidence of deep vein thrombosis (DVT) or blood clots in the lungs at 30-70% for COVID patients admitted to the ICU.
Prior to the pandemic, advocacy efforts were already under way to treat varicose veins and other venous insufficiencies to prevent exacerbating other health problems. Post-operative blood clots have been realized as one of the top preventable causes of death in hospitalized patients.
Treating the underlying conditions that may cause these clots, prior to surgery, has been recognized as a critical step for patient success. In fact, some surgeons are now mandating screenings and treatment for varicose veins and venous insufficiency prior to surgery for other medical conditions.
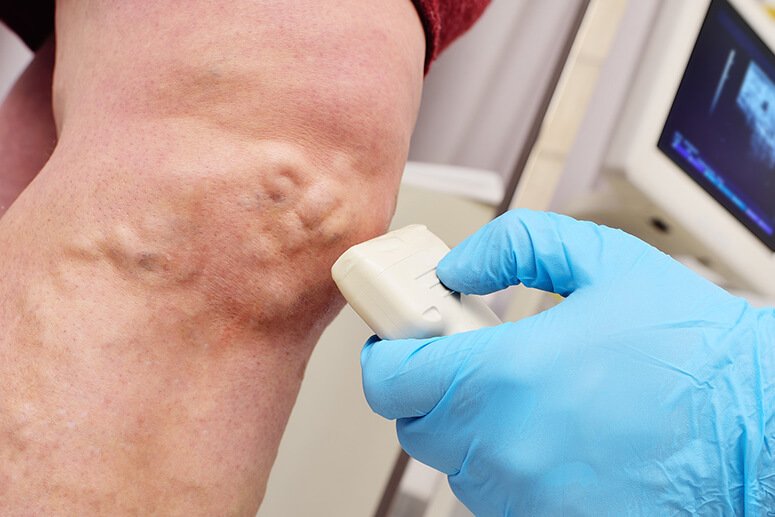
The same pre-emptive measures are advisable in the era of coronavirus. It is important to reduce factors commonly known to cause significant risk of blood clotting, stroke, and pulmonary embolism. Infection from COVID-19 can raise the risk substantially for patients with untreated vascular diseases.
Identifying and treating the symptoms of COVID-19 is also challenging in the presence of venous insufficiency. For example, lung issues associated with the virus present similarly to the symptoms of pulmonary embolism, making the distinction between them difficult to assess.
Diabetes can complicate matters further. While the connection between varicose veins and diabetes is indirect, they share some risk factors related to blood circulation. Coronavirus compounds the problem further. According to the CDC “having either type 1 or type 2 diabetes can make you more likely to get severely ill from COVID-19.”
Patients with diabetes should consult with a board-certified vascular surgeon to see if they have underlying venous issues. Pre-emptive screening and treatment for venous insufficiency should be considered, with or without the risk of COVID-19 infection.
A recent study has shown that a higher risk of blood clots exists for patients who contracted COVID-19 as far back as twelve months. This risk carries even to those who were not hospitalized. Further, these risks extend into a wide range of cardiovascular disease such as ischemic heart disease, heart failure, and venous thromboembolism (VTE).
There is no doubt that the risks associated with COVID-19 will continue to be researched and assessed into the future. While proactive diagnosis and treatment for vascular disease is always advisable, it takes on even more urgency in the coronavirus era. If you suspect or are aware of vascular problems, immediate consultation with a board-certified vascular surgeon is highly recommended to maintain optimal health.
Written in conjunction with Coastal Vein and Vascular Specialists in Palm Beach Gardens, Florida. This award-winning team of practitioners is committed to excellence in vascular medical care with renown for treating the most complex vascular disorders.
Resources
What Does COVID Do to Your Blood?; Johns Hopkins Medicine
https://www.hopkinsmedicine.org/health/conditions-and-diseases/coronavirus/what-does-covid-do-to-your-blood
People With Coronavirus Are At Risk Of Blood Clots And Strokes; Heart Research Institute
https://www.hri.org.au/health/your-health/lifestyle/people-with-coronavirus-are-at-risk-of-blood-clots-and-strokes
COVID-19: People with Certain Medical Conditions; Centers for Disease Control and Prevention
https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/people-with-medical-conditions.html (see Diabetes, Heart Conditions)